EP4008263B1 - Verfahren zur subkutanen gewebedickenmessung, gerät und vorrichtung sowie speichermedium - Google Patents
Verfahren zur subkutanen gewebedickenmessung, gerät und vorrichtung sowie speichermedium Download PDFInfo
- Publication number
- EP4008263B1 EP4008263B1 EP20847157.3A EP20847157A EP4008263B1 EP 4008263 B1 EP4008263 B1 EP 4008263B1 EP 20847157 A EP20847157 A EP 20847157A EP 4008263 B1 EP4008263 B1 EP 4008263B1
- Authority
- EP
- European Patent Office
- Prior art keywords
- subcutaneous tissue
- ultrasonic
- moment
- ultrasonic echo
- echo signals
- Prior art date
- Legal status (The legal status is an assumption and is not a legal conclusion. Google has not performed a legal analysis and makes no representation as to the accuracy of the status listed.)
- Active
Links
Images
Classifications
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/08—Clinical applications
- A61B8/0833—Clinical applications involving detecting or locating foreign bodies or organic structures
- A61B8/085—Clinical applications involving detecting or locating foreign bodies or organic structures for locating body or organic structures, e.g. tumours, calculi, blood vessels, nodules
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/08—Clinical applications
- A61B8/0858—Clinical applications involving measuring tissue layers, e.g. skin, interfaces
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/42—Details of probe positioning or probe attachment to the patient
- A61B8/4245—Details of probe positioning or probe attachment to the patient involving determining the position of the probe, e.g. with respect to an external reference frame or to the patient
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/52—Devices using data or image processing specially adapted for diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/5215—Devices using data or image processing specially adapted for diagnosis using ultrasonic, sonic or infrasonic waves involving processing of medical diagnostic data
- A61B8/5223—Devices using data or image processing specially adapted for diagnosis using ultrasonic, sonic or infrasonic waves involving processing of medical diagnostic data for extracting a diagnostic or physiological parameter from medical diagnostic data
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B8/00—Diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/52—Devices using data or image processing specially adapted for diagnosis using ultrasonic, sonic or infrasonic waves
- A61B8/5269—Devices using data or image processing specially adapted for diagnosis using ultrasonic, sonic or infrasonic waves involving detection or reduction of artifacts
Definitions
- the present invention relates to the technical field of measurement of thickness of subcutaneous tissues, in particular to a method, apparatus and device for measuring a thickness of a subcutaneous tissue and a storage medium.
- Drug administration to patients includes oral administration and injection. Drug administration is determined in consideration of the purpose of the drug administration, patient health factors, and the like. In the case of injection, a region of the body where injection is to be performed may be determined based on the purpose of drug administration, patient health factors, and the like.
- Diabetic patients require periodic insulin administration, which is performed by injection. Insulin is most often injected subcutaneously, and is primarily injected into the abdomen, the arms, the thighs, the buttocks, and other parts of the body.
- Subcutaneous tissues are loose connective tissue and adipose tissue beneath the skin which connect the skin to the muscles. Since the subcutaneous tissues are located between the skin and the muscles, a too short injection needle may cause insulin to be administered to the skin, while a too long injection needle may cause insulin to be administered to the muscles. Therefore, although it may be necessary to select an appropriate injection needle length in accordance with the thickness of the subcutaneous tissues, the impossibility of observing the thickness of the subcutaneous tissues prohibits safe and effective insulin supply. How to accurately measure the thickness of the subcutaneous tissues has become an urgent technical problem to be solved.
- WO 2018/029035 A1 discloses a system and method for determining fat and lean body tissue components. The journal paper " Pattern recognition on human skin tissue" by A. Pech et al. in Acoustical Imaging, Vol. 18, of Plenum Press, New York, 1991 , discloses a method for examining human skin tissue.
- the present invention provides a method, apparatus and device for measuring a thickness of a subcutaneous tissue and a storage medium, which are used for accurately measuring the thickness of the subcutaneous tissues.
- One aspect of the present invention provides a method according to claim 1.
- Another aspect of the present invention provides an apparatus according to claim 7.
- Another aspect of the present invention provides a computer-readable storage medium having a computer program stored therein, according to claim 13.
- FIG. 1 is a flowchart of a method for measuring a thickness of a subcutaneous tissue according to Embodiment 1 of the present invention. As shown in FIG. 1 , the method includes the following specific steps:
- the moment the ultrasonic detector emits the ultrasonic detection waves and the received ultrasonic echo signals generated by the ultrasonic detection waves passing through the subcutaneous tissue and the deep fascia layer can be acquired.
- the ultrasonic parameter includes at least one of: scattering peak, scatterer density, scatterer distribution characteristic, reflectance value, reflectance value distribution, etc.
- the ultrasonic parameter may also be other parameters that can reflect different reflection or transmission characteristics of the subcutaneous tissue and the deep fascia layer to the ultrasonic detection waves, which is not specifically limited by this embodiment here.
- the characteristic parameter threshold of the subcutaneous tissue is used to indicate the reflection or transmission characteristic of the subcutaneous tissue, and may be set by a skilled person according to a large number of experimental results and experiences, which is not specifically limited by this embodiment here.
- the ultrasonic echo signals meeting the characteristic parameter threshold of the subcutaneous tissue and the ultrasonic echo signals not meeting the characteristic parameter threshold of the subcutaneous tissue may be separated according to the ultrasonic parameter values of the ultrasonic echo signals of the ultrasonic detection waves, so that the ultrasonic echo signals of the subcutaneous tissue can be obtained and the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received can be further determined.
- the distance from the surface of the ultrasonic detector to the boundary of the subcutaneous tissue is the thickness of the subcutaneous tissue.
- S103 calculating a thickness of the subcutaneous tissue according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- a time interval from the emission of the ultrasonic detection waves to the reception of the ultrasonic echo signals from the boundary of the subcutaneous tissue can be calculated, and according to the time interval and the speed of the ultrasonic echo signals propagating in the subcutaneous tissue, a thickness value of the subcutaneous tissue can be calculated.
- ultrasonic detection waves are emitted inwards from a skin surface by an ultrasonic detector, and ultrasonic echo signals of the ultrasonic detection waves are received; the moment the ultrasonic echo signals from the boundary of a subcutaneous tissue are received is determined according to ultrasonic parameter values of the ultrasonic echo signals and a characteristic parameter threshold of the subcutaneous tissue; a thickness of the subcutaneous tissue is calculated according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received, and thereby the thickness of the subcutaneous tissue can be accurately measured.
- FIG. 2 is a flowchart of a method for measuring a thickness of a subcutaneous tissue according to Embodiment 2 of the present invention.
- the method further includes correcting the calculated thickness of the subcutaneous tissue. As shown in FIG. 2 , the method includes the following specific steps:
- the ultrasonic parameter is any of: scattering peak, scatterer density, scatterer distribution characteristic, reflectance value, reflectance value distribution, etc.
- the ultrasonic parameter may also be other parameters that can reflect different reflection or transmission characteristics of the subcutaneous tissue and the deep fascia layer to the ultrasonic detection waves, which is not specifically limited by this embodiment here.
- the characteristic parameter threshold of the subcutaneous tissue includes a first threshold, which is used to indicate the reflection or transmission characteristic of the subcutaneous tissue, and may be set by a skilled person according to a large number of experimental results and experiences, which is not specifically limited by this embodiment here.
- the ultrasonic echo signals meeting the characteristic parameter threshold of the subcutaneous tissue and the ultrasonic echo signals not meeting the characteristic parameter threshold of the subcutaneous tissue may be separated according to the ultrasonic parameter values of the ultrasonic echo signals of the ultrasonic detection waves, so that the ultrasonic echo signals of the subcutaneous tissue can be obtained and the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received can be further determined.
- the distance from the surface of the ultrasonic detector to the boundary of the subcutaneous tissue is the thickness of the subcutaneous tissue.
- the determining, according to ultrasonic parameter values of the ultrasonic echo signals and a characteristic parameter threshold of the subcutaneous tissue, the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received may specifically be implemented by adopting the following steps: Step 1: After the ultrasonic detection waves are emitted, a first mean of ultrasonic parameter values of N consecutive ultrasonic echo signals starting from the first ultrasonic echo signal received are calculated.
- Step 2 is repeated until a first mean of ultrasonic parameter values of a group of N consecutive ultrasonic echo signals acquired is greater than the first threshold value. If the first mean is greater than the first threshold value, Step 3 is executed.
- Step 2 A next group of N consecutive ultrasonic echo signals are acquired, and a first mean of ultrasonic parameter values of the group of N consecutive ultrasonic echo signals is calculated.
- Step 3 If the first mean is greater than the first threshold value, the N ultrasonic echo signals are taken as a first group of signals, and a second mean of ultrasonic parameter values of N consecutive ultrasonic echo signals following the first group of signals is calculated.
- Step 2 is executed to acquire a next group of N consecutive ultrasonic echo signals.
- Step 4 If the second mean is less than the second threshold value, the moment the last ultrasonic echo signal in the first group of signals is received is determined as a first moment of reception, and the moment a first ultrasonic echo signal following the first group of signals is received is determined as a second moment of reception; and an intermediate moment between the first moment of reception and the second moment of reception is determined as the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- N is a positive integer, and the value of N may be set by a skilled person according to a large number of experimental results and experiences. For example, the value of N may be set within an interval [1,20], which is not specifically limited by this embodiment here.
- N may be 5. If a mean of scattering peaks of ultrasonic echo signals received over a period of five consecutive moments is greater than the first threshold and a mean of scattering peaks of ultrasonic echo signals received over a period of five consecutive moments following the five moments is less than the second threshold, an intermediate moment between the last moment in the former group of five consecutive moments and the first moment in the latter group of five consecutive moments is taken as the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received, so that the boundary of the subcutaneous tissue can be determined, and the distance from the skin surface where the ultrasonic detector is located to the boundary of the subcutaneous tissue is the thickness of the subcutaneous tissue.
- the first threshold and the second threshold may be set by a skilled person according to a large number of experimental results and experiences, which is not specifically limited by this embodiment here.
- S203 calculating a thickness of the subcutaneous tissue according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received; In this embodiment, this step may be specifically implemented in the following way:
- a propagation duration of the ultrasonic echo signals from the boundary of the subcutaneous tissue is determined according to the moment of emitting the ultrasonic detection waves and the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received; and the thickness of the subcutaneous tissue is calculated according to the propagation duration of the ultrasonic echo signals from the boundary of the subcutaneous tissue and the propagation speed of the ultrasonic echo signals in the subcutaneous tissue.
- S204 adding the calculated thickness of the subcutaneous tissue to the length of a measurement blind area of the ultrasonic detector to correct the calculated thickness of the subcutaneous tissue;
- the ultrasonic detector has a certain measurement blind area when performing measurement, errors will be brought to the measurement of the thickness of the subcutaneous tissue.
- the calculated thickness of the subcutaneous tissue may be corrected according to the length of the measurement blind area of the ultrasonic detector.
- a sum of the thickness of the subcutaneous tissue and the length of the measurement blind area of the ultrasonic detector is calculated according to the currently obtained thickness of the subcutaneous tissue, and the sum of the thickness of the subcutaneous tissue and the length of the measurement blind area of the ultrasonic detector is taken as a corrected thickness value of the subcutaneous tissue.
- S205 subtracting the length of a matching layer of the ultrasonic detector from the calculated thickness of the subcutaneous tissue to correct the calculated thickness of the subcutaneous tissue;
- the ultrasonic detector includes a piezoelectric layer in which a piezoelectric material vibrates to perform conversion between electrical signals and acoustic signals.
- the matching layer reduces an acoustic impedance difference between the piezoelectric layer and the object so as to transmit ultrasonic waves generated from the piezoelectric layer to the object to the maximum.
- the calculated thickness of the subcutaneous tissue may be corrected according to the length of the matching layer of the ultrasonic detector.
- a difference obtained by subtracting the length of the matching layer of the ultrasonic detector from the thickness of the subcutaneous tissue is calculated and taken as a corrected thickness value of the subcutaneous tissue.
- the ultrasonic detector presses the skin surface, and as a result, the skin is sunk inwards by a certain depth (i.e., the pressing depth) under the action of pressure, brining errors to the measurement of the thickness of the subcutaneous tissue.
- the calculated thickness of the subcutaneous tissue may be corrected according to the pressing depth of the ultrasonic detector on the skin surface.
- the adding the calculated thickness of the subcutaneous tissue to a pressing depth of the ultrasonic detector to correct the calculated thickness of the subcutaneous tissue may be specifically implemented in the following way:
- a pressing depth of the ultrasonic detector on the skin surface is acquired; a sum of the thickness of the subcutaneous tissue and the pressing depth is calculated and taken as a corrected thickness of the subcutaneous tissue.
- the pressing depth of the ultrasonic detector on the skin surface may be acquired in the following way:
- the pressing depth of the ultrasonic detector on the skin surface may be determined through measurement information of a sensor, such as a pressure sensor, a displacement sensor, or a position sensor; or, according to data collected during the period from the time when the ultrasonic detector is placed on the skin surface until the pressing is stabilized, an accumulated deformation degree of the tissue is calculated using a block matching method (such as cross correlation or autocorrelation), a filtering method or the like, obtaining the pressing depth.
- a sensor such as a pressure sensor, a displacement sensor, or a position sensor
- an accumulated deformation degree of the tissue is calculated using a block matching method (such as cross correlation or autocorrelation), a filtering method or the like, obtaining the pressing depth.
- the method for acquiring the pressing depth of the ultrasonic detector on the skin surface may also be implemented by using any method for determining a pressing depth of an ultrasonic detector in the process of measurement in the prior art, which is not specifically limited by this embodiment here.
- the calculated thickness of the subcutaneous tissue is corrected according to to-be-corrected contents of the ultrasonic detector.
- the ultrasonic detector may be an ultrasonic probe, in which case a measurement blind area formed by the morphology of the ultrasonic probe, a matching layer of the ultrasonic probe, etc. should be taken into consideration.
- the calculated thickness value of the subcutaneous tissue may also be corrected according to one or more correction value among a measurement blind area length and matching layer length of the ultrasonic detector and the pressing depth of the ultrasonic detector on the skin surface during measurement, so as to increase the accuracy of the finally measured thickness of the subcutaneous tissue.
- the thickness of the subcutaneous tissue may also be corrected according to other factors affecting the measurement of the thickness of the subcutaneous tissue, which is not specifically limited by this embodiment here.
- correction can be performed once according to the at least two correction values; or, as shown in S204 to S206 above, the calculated thickness of the subcutaneous tissue is corrected multiple times according to different correction values, and in this case, since the correction using each correction value is independent, the order of correction based on each correction value is not limited.
- S204 to S206 above in this embodiment are only illustrative, and in other embodiments, correction may be performed in other ways, which is not specifically limited by this embodiment here.
- a first mean of ultrasonic parameter values of N consecutive ultrasonic echo signals starting from the first ultrasonic echo signal received is calculated, with N being a positive integer; if the first mean is greater than a first threshold value, the N ultrasonic echo signals are taken as a first group of signals, and a second mean of ultrasonic parameter values of N consecutive ultrasonic echo signals following the first group of signals are calculated; if the second mean is less than a second threshold value, a first moment of reception of the last ultrasonic echo signal in the first group of signals and a second moment of reception of a first ultrasonic echo signal following the first group of signals are determined; and an intermediate moment between the first moment of reception and the second moment of reception is determined as the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received can be accurately determined, laying a foundation for the obtainment of the accurate thickness of the subcutaneous tissue.
- the obtained thickness of the subcutaneous tissue can be corrected according to the measurement blind area length and matching layer length of the ultrasonic detector and the pressing depth of the ultrasonic detector on the skin surface during measurement, increasing the accuracy of the measurement of the thickness of the subcutaneous tissue.
- FIG. 3 is a schematic structural diagram of an apparatus for measuring a thickness of a subcutaneous tissue according to Embodiment 3 of the present invention.
- the apparatus for measuring a thickness of a subcutaneous tissue provided by the embodiment of the present invention can execute the processing flows provided by the method embodiments for measuring a thickness of a subcutaneous tissue.
- the apparatus 30 for measuring a thickness of a subcutaneous tissue includes: a measuring module 301, a boundary determination module 302, and a thickness calculation module 303.
- the measuring module 301 is configured for emitting ultrasonic detection waves inwards from a skin surface and acquiring ultrasonic echo signals of the ultrasonic detection waves.
- the boundary determination module 302 is configured for determining, according to ultrasonic parameter values of the ultrasonic echo signals and a characteristic parameter threshold of a subcutaneous tissue, the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- the thickness calculation module 303 is configured for calculating a thickness of the subcutaneous tissue according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- the apparatus provided by the embodiment of the present invention can be specifically used to execute the method embodiment provided by Embodiment 1 described above, and specific functions will not be described here again.
- ultrasonic detection waves are emitted inwards from a skin surface by an ultrasonic detector, and ultrasonic echo signals of the ultrasonic detection waves are received; the moment the ultrasonic echo signals from the boundary of a subcutaneous tissue are received is determined according to ultrasonic parameter values of the ultrasonic echo signals and a characteristic parameter threshold of the subcutaneous tissue; a thickness of the subcutaneous tissue is calculated according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received, and thereby the thickness of the subcutaneous tissue can be accurately measured.
- the ultrasonic parameter is any of: scattering peak, scatterer density, scatterer distribution characteristic, reflectance value and reflectance value distribution.
- the boundary determination module is further configured for: calculating a first mean of ultrasonic parameter values of N consecutive ultrasonic echo signals starting from the first ultrasonic echo signal received after the ultrasonic detection waves are emitted, with N being a positive integer; if the first mean is greater than a first threshold value, taking the N ultrasonic echo signals as a first group of signals, and calculating a second mean of ultrasonic parameter values of N consecutive ultrasonic echo signals following the first group of signals; if the second mean is less than a second threshold value, determining the moment the last ultrasonic echo signal in the first group of signals is received as a first moment of reception and the moment a first ultrasonic echo signal following the first group of signals is received as a second moment of reception; and determining an intermediate moment between the first moment of reception and the second moment of reception as the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- the thickness calculation module is further configured for: determining a propagation duration of the ultrasonic echo signals from the boundary of the subcutaneous tissue according to the moment of emitting the ultrasonic detection waves and the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received; and calculating the thickness of the subcutaneous tissue according to the propagation duration of the ultrasonic echo signals from the boundary of the subcutaneous tissue and the propagation speed of the ultrasonic echo signals in the subcutaneous tissue.
- the thickness calculation module is further configured for: adding the calculated thickness of the subcutaneous tissue to the length of a measurement blind area of the ultrasonic detector to correct the calculated thickness of the subcutaneous tissue.
- the thickness calculation module is further configured for: subtracting the length of a matching layer of the ultrasonic detector from the calculated thickness of the subcutaneous tissue to correct the calculated thickness of the subcutaneous tissue.
- the thickness calculation module is further configured for: acquiring a pressing depth of the ultrasonic detector on the skin surface; and adding the pressing depth to the calculated thickness of the subcutaneous tissue to correct the calculated thickness of the subcutaneous tissue.
- the apparatus provided by the embodiment of the present invention can be specifically used to execute the method embodiment provided by Embodiment 2 described above, and specific functions will not be described here again.
- a first mean of ultrasonic parameter values of N consecutive ultrasonic echo signals starting from the first ultrasonic echo signal received is calculated, with N being a positive integer; if the first mean is greater than a first threshold value, the N ultrasonic echo signals are taken as a first group of signals, and a second mean of ultrasonic parameter values of N consecutive ultrasonic echo signals following the first group of signals is calculated; if the second mean is less than a second threshold value, the moment the last ultrasonic echo signal in the first group of signals is received is determined as a first moment of reception, and the moment a first ultrasonic echo signal following the first group of signals is received is determined as a second moment of reception; and an intermediate moment between the first moment of reception and the second moment of reception is determined as the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received.
- the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received can be accurately determined, laying a foundation for the obtainment of the accurate thickness of the subcutaneous tissue.
- the obtained thickness of the subcutaneous tissue can be corrected according to the measurement blind area length and matching layer length of the ultrasonic detector and the pressing depth of the ultrasonic detector on the skin surface during measurement, increasing the accuracy of the measurement of the thickness of the subcutaneous tissue.
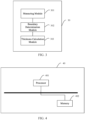
- FIG. 4 is a schematic structural diagram of a device for measuring a thickness of a subcutaneous tissue according to Embodiment 5 of the present invention.
- the device 40 for measuring a thickness of a subcutaneous tissue includes: a processor 401, a memory 402, and a computer program stored in the memory 402 and executable by the processor 401.
- the processor 401 implements the method for measuring subcutaneous tissue thickness provided by any of the method embodiments described above when executing the computer program stored in the memory 402.
- ultrasonic detection waves are emitted inwards from a skin surface by an ultrasonic detector, and ultrasonic echo signals of the ultrasonic detection waves are received; the moment the ultrasonic echo signals from the boundary of a subcutaneous tissue are received is determined according to ultrasonic parameter values of the ultrasonic echo signals and a characteristic parameter threshold of the subcutaneous tissue; a thickness of the subcutaneous tissue is calculated according to the moment the ultrasonic echo signals from the boundary of the subcutaneous tissue are received, and thereby the thickness of the subcutaneous tissue can be accurately measured.
- an embodiment of the present invention further provides a computer-readable storage medium having a computer program stored therein, wherein the computer program implements the method for measuring a thickness of a subcutaneous tissue provided by any of the method embodiments described above when executed by a processor.
- the disclosed apparatus and method may be implemented in other ways.
- the above-described apparatus embodiments are merely illustrative, and for example, the division of the units is only a logical function division.
- Other division methods may be implemented in practice, for example, a plurality of units or components may be combined or integrated into another system, or some features may be omitted, or not executed.
- mutual coupling or direct coupling or communication connection shown or discussed may be indirect coupling or communication connection through some interfaces, apparatuses or units, or may be in electrical, mechanical or other forms.
- the units described as separate parts may or may not be physically separated, and parts shown as units may or may not be physical units, that is, they may be located at one position or distributed on a plurality of network units. Some or all of the units can be selected according to actual needs to achieve the purpose of the solution of the embodiment.
- functional units in the embodiments of the present invention may be integrated into one processing unit, or each unit may exist alone physically, or two or more units may be integrated into one unit.
- the aforementioned integrated unit may be implemented in the form of hardware or in the form of hardware plus a functional software unit.
- the aforementioned integrated unit implemented in the form of the functional software unit may be stored in a computer-readable storage medium.
- the aforementioned functional software unit is stored in a storage medium and includes several instructions for causing a computer device (e.g., a personal computer, a server or a network device) or a processor to execute some steps of the method according to each embodiment of the present invention.
- the aforementioned storage medium includes: a USB flash disk, a mobile hard disk, a read-only memory (ROM), a random access memory (RAM), a magnetic disk, an optical disk, or other various media capable of storing program codes.
Landscapes
- Health & Medical Sciences (AREA)
- Life Sciences & Earth Sciences (AREA)
- Engineering & Computer Science (AREA)
- Biomedical Technology (AREA)
- Medical Informatics (AREA)
- Veterinary Medicine (AREA)
- Biophysics (AREA)
- Nuclear Medicine, Radiotherapy & Molecular Imaging (AREA)
- Pathology (AREA)
- Radiology & Medical Imaging (AREA)
- Public Health (AREA)
- Heart & Thoracic Surgery (AREA)
- Physics & Mathematics (AREA)
- Molecular Biology (AREA)
- Surgery (AREA)
- Animal Behavior & Ethology (AREA)
- General Health & Medical Sciences (AREA)
- Computer Vision & Pattern Recognition (AREA)
- Physiology (AREA)
- Vascular Medicine (AREA)
- Ultra Sonic Daignosis Equipment (AREA)
- Length Measuring Devices Characterised By Use Of Acoustic Means (AREA)
Claims (13)
- Verfahren zur Messung der Dicke von subkutanem Gewebe, dadurch gekennzeichnet, dass es umfasst:Senden einer Ultraschalldetektionswelle von der Hautoberfläche nach innen und Erfassen eines Ultraschallechosignals der Ultraschalldetektionswelle (S101);Bestimmen eines Empfangszeitpunkts eines Ultraschallechosignals an der Grenze des subkutanen Gewebes auf der Grundlage eines Werts eines Ultraschallparameters des Ultraschallechosignals und eines Schwellenwerts eines charakteristischen Parameters des subkutanen Gewebes (S102);Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes (S103),wobei das Bestimmen eines Empfangszeitpunkts eines Ultraschallechosignals an der Grenze des subkutanen Gewebes auf der Grundlage eines Werts eines Ultraschallparameters des Ultraschallechosignals und eines Schwellenwerts eines charakteristischen Parameters des subkutanen Gewebes umfasst:nach dem Senden der Ultraschalldetektionswelle, beginnend mit einem ersten empfangenen Ultraschallechosignal, Berechnen eines ersten Mittelwerts der Werte des Ultraschallparameters von aufeinanderfolgenden N Ultraschallechosignalen, wobei N eine positive ganze Zahl ist,wenn der erste Mittelwert größer als ein erster Schwellenwert ist, Betrachten der N Ultraschallechosignale als eine erste Gruppe von Signalen und Berechnen eines zweiten Mittelwerts der Werte des Ultraschallparameters der aufeinanderfolgenden N Ultraschallechosignale im Anschluss an die erste Gruppe von Signalen,wenn der zweite Mittelwert kleiner als ein zweiter Schwellenwert ist, Bestimmen des Empfangszeitpunkts des letzten Ultraschallechosignals in der ersten Gruppe von Signalen als ein erster Empfangszeitpunkt und des Empfangszeitpunkts des ersten Ultraschallechosignals im Anschluss an die erste Gruppe von Signalen als ein zweiter Empfangszeitpunkt; undBestimmen eines Zwischenzeitpunkts zwischen dem ersten Empfangszeitpunkt und dem zweiten Empfangszeitpunkt als ein Empfangszeitpunkt des Ultraschallechosignals an der Grenze des subkutanen Gewebes.
- Verfahren nach Anspruch 1, dadurch gekennzeichnet, dass der Ultraschallparameter mindestens einen der folgenden Parameter umfasst:
Streuspitze, Streudichte, Streuverteilungsmerkmale, Reflexionswert und Reflexionswertverteilung. - Verfahren nach Anspruch 1, dadurch gekennzeichnet, dass das Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes umfasst:Bestimmen einer Ausbreitungszeit des Ultraschallechosignals an der Grenze des subkutanen Gewebes auf der Grundlage des Sendezeitpunkts der Ultraschalldetektionswelle und des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes,Berechnen der Dicke des subkutanen Gewebes auf der Grundlage der Ausbreitungszeit des Ultraschallechosignals an der Grenze des subkutanen Gewebes und einer Ausbreitungsgeschwindigkeit des Ultraschallechosignals im subkutanen Gewebe.
- Verfahren nach einem der Ansprüche 1 bis 3, dadurch gekennzeichnet, dass es nach dem Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes ferner umfasst
Addieren der berechneten Dicke des subkutanen Gewebes zu einer Länge eines Messblindbereichs einer Ultraschalldetektionsvorrichtung, um die berechnete Dicke des subkutanen Gewebes zu korrigieren. - Verfahren nach einem der Ansprüche 1 bis 3, dadurch gekennzeichnet, dass es nach dem Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes ferner umfasst:
Subtrahieren einer Länge einer Anpassungsschicht der Ultraschalldetektionsvorrichtung von der berechneten Dicke des subkutanen Gewebes, um die berechnete Dicke des subkutanen Gewebes zu korrigieren. - Verfahren nach einem der Ansprüche 1 bis 3, dadurch gekennzeichnet, dass es nach dem Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes ferner umfasst:Ermitteln einer Eindrücktiefe der Ultraschalldetektionsvorrichtung auf der Hautoberfläche;Addieren der berechneten Dicke des subkutanen Gewebes zu der Eindrücktiefe, um die berechnete Dicke des subkutanen Gewebes zu korrigieren.
- Vorrichtung zur Messung der Dicke von subkutanem Gewebe, dadurch gekennzeichnet, dass sie umfasst:ein Messmodul (301) zum Senden einer Ultraschalldetektionswelle von der Hautoberfläche nach innen und Erfassen eines Ultraschallechosignals der Ultraschalldetektionswelle,ein Grenzbestimmungsmodul (302) zum Bestimmen eines Empfangszeitpunkts eines Ultraschallechosignals an der Grenze des subkutanen Gewebes auf der Grundlage eines Werts eines Ultraschallparameters des Ultraschallechosignals undeines Schwellenwerts eines charakteristischen Parameters des subkutanen Gewebes,ein Dickenberechnungsmodul (303) zum Berechnen einer Dicke des subkutanen Gewebes auf der Grundlage des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes,wobei das Grenzbestimmungsmodul auch dazu verwendet wird:nach dem Senden der Ultraschalldetektionswelle, beginnend mit einem ersten empfangenen Ultraschallechosignal, einen ersten Mittelwert der Werte des Ultraschallparameters von aufeinanderfolgenden N Ultraschallechosignalen zu berechnen, wobei N eine positive ganze Zahl ist,wenn der erste Mittelwert größer als ein erster Schwellenwert ist, die N Ultraschallechosignale als eine erste Gruppe von Signalen zu betrachten und einen zweiten Mittelwert der Werte des Ultraschallparameters der aufeinanderfolgenden N Ultraschallechosignale im Anschluss an die erste Gruppe von Signalen zu berechnen,wenn der zweite Mittelwert kleiner als ein zweiter Schwellenwert ist, den Empfangszeitpunkt des letzten Ultraschallechosignals in der ersten Gruppe von Signalen als einen ersten Empfangszeitpunkt und den Empfangszeitpunkt des ersten Ultraschallechosignals im Anschluss an die erste Gruppe von Signalen, als einen zweiten Empfangszeitpunkt zu bestimmen; undeinen Zwischenzeitpunkt zwischen dem ersten Empfangszeitpunkt und dem zweiten Empfangszeitpunkt als einen Empfangszeitpunkt des Ultraschallechosignals an der Grenze des subkutanen Gewebes zu bestimmen.
- Vorrichtung nach Anspruch 7, dadurch gekennzeichnet, dass der Ultraschallparameter mindestens einen der folgenden Parameter umfasst:
Streuspitze, Streudichte, Streuverteilungsmerkmale, Reflexionswert und Reflexionswertverteilung. - Vorrichtung nach Anspruch 7, dadurch gekennzeichnet, dass das Dickenberechnungsmodul auch dazu verwendet wird:eine Ausbreitungszeit des Ultraschallechosignals an der Grenze des subkutanen Gewebes auf der Grundlage des Sendezeitpunkts der Ultraschalldetektionswelle und des Empfangszeitpunkts des Ultraschallechosignals an der Grenze des subkutanen Gewebes zu bestimmen;die Dicke des subkutanen Gewebes auf der Grundlage der Ausbreitungszeit des Ultraschallechosignals an der Grenze des subkutanen Gewebes und einer Ausbreitungsgeschwindigkeit des Ultraschallechosignals im subkutanen Gewebe zu berechnen.
- Vorrichtung nach einem der Ansprüche 7 bis 9, dadurch gekennzeichnet, dass das Dickenberechnungsmodul auch dazu verwendet wird:
die berechnete Dicke des subkutanen Gewebes zu einer Länge eines Messblindbereichs einer Ultraschalldetektionsvorrichtung zu addieren, um die berechnete Dicke des subkutanen Gewebes zu korrigieren. - Vorrichtung nach einem der Ansprüche 7 bis 9, dadurch gekennzeichnet, dass das Dickenberechnungsmodul auch dazu verwendet wird:
eine Länge einer Anpassungsschicht der Ultraschalldetektionsvorrichtung von der berechneten Dicke des subkutanen Gewebes zu subtrahieren, um die berechnete Dicke des subkutanen Gewebes zu korrigieren. - Vorrichtung nach einem der Ansprüche 7 bis 9, dadurch gekennzeichnet, dass das Dickenberechnungsmodul auch dazu verwendet wird:eine Eindrücktiefe der Ultraschalldetektionsvorrichtung auf der Hautoberfläche zu ermitteln;die berechnete Dicke des subkutanen Gewebes zu der Eindrücktiefe zu addieren, um die berechnete Dicke des subkutanen Gewebes zu korrigieren.
- Computerlesbares Speichermedium, dadurch gekennzeichnet, dass es ein Computerprogramm speichert,
wobei das Computerprogramm, wenn es von einem Prozessor ausgeführt wird, ein Verfahren nach einem der Ansprüche 1 bis 6 implementiert.
Applications Claiming Priority (2)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| CN201910706602.1A CN110313938B (zh) | 2019-08-01 | 2019-08-01 | 皮下组织厚度测量方法、装置、设备及存储介质 |
| PCT/CN2020/105022 WO2021018108A1 (zh) | 2019-08-01 | 2020-07-28 | 皮下组织厚度测量方法、装置、设备及存储介质 |
Publications (4)
| Publication Number | Publication Date |
|---|---|
| EP4008263A1 EP4008263A1 (de) | 2022-06-08 |
| EP4008263A4 EP4008263A4 (de) | 2023-01-25 |
| EP4008263B1 true EP4008263B1 (de) | 2024-09-04 |
| EP4008263C0 EP4008263C0 (de) | 2024-09-04 |
Family
ID=68123429
Family Applications (1)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| EP20847157.3A Active EP4008263B1 (de) | 2019-08-01 | 2020-07-28 | Verfahren zur subkutanen gewebedickenmessung, gerät und vorrichtung sowie speichermedium |
Country Status (6)
| Country | Link |
|---|---|
| US (1) | US12290399B2 (de) |
| EP (1) | EP4008263B1 (de) |
| JP (1) | JP7249711B2 (de) |
| CN (1) | CN110313938B (de) |
| BR (1) | BR112022001734A2 (de) |
| WO (1) | WO2021018108A1 (de) |
Families Citing this family (6)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| CN204637350U (zh) | 2013-03-08 | 2015-09-16 | 奥赛拉公司 | 美学成像与处理系统、多焦点处理系统和执行美容过程的系统 |
| WO2020112688A1 (en) | 2018-11-30 | 2020-06-04 | Ulthera, Inc. | Systems and methods for enhancing efficacy of ultrasound treatment |
| CN110313938B (zh) * | 2019-08-01 | 2021-03-23 | 无锡海斯凯尔医学技术有限公司 | 皮下组织厚度测量方法、装置、设备及存储介质 |
| US20230301622A1 (en) * | 2020-08-13 | 2023-09-28 | Otago Innovation Limited | Dental device and methods |
| CN114428527A (zh) * | 2022-01-26 | 2022-05-03 | 云南贝泰妮生物科技集团股份有限公司 | 一种基于超声回波的射频美容仪温控系统 |
| CN116584975B (zh) * | 2023-04-03 | 2025-10-10 | 无锡海斯凯尔医学技术有限公司 | 皮下组织厚度测量方法、装置、电子设备及存储介质 |
Family Cites Families (18)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| JP2840040B2 (ja) * | 1994-12-22 | 1998-12-24 | アロカ株式会社 | 組織内音速測定方法 |
| JP3563904B2 (ja) | 1996-12-16 | 2004-09-08 | ジーイー横河メディカルシステム株式会社 | 超音波診断装置および壁厚計測方法 |
| US8162837B2 (en) * | 2005-06-13 | 2012-04-24 | Spentech, Inc. | Medical doppler ultrasound system for locating and tracking blood flow |
| CN101527047B (zh) | 2008-03-05 | 2013-02-13 | 深圳迈瑞生物医疗电子股份有限公司 | 使用超声图像检测组织边界的方法与装置 |
| WO2012014192A2 (en) * | 2010-07-25 | 2012-02-02 | Syneron Medical Ltd. | A method and apparatus for measuring the thickness of adipose tissue |
| CN103429163B (zh) * | 2011-01-05 | 2015-07-08 | 皇家飞利浦电子股份有限公司 | 用于确定身体的实际组织层边界的装置和方法 |
| CN103126726B (zh) * | 2011-11-25 | 2015-03-04 | 重庆海扶医疗科技股份有限公司 | 一种脂肪厚度测量装置 |
| CN102636252B (zh) | 2012-04-10 | 2013-11-27 | 吉林大学 | 一种超声波到达精确时刻检测的方法及装置 |
| US11259779B2 (en) | 2014-12-26 | 2022-03-01 | Furuno Electric Co., Ltd. | Ultrasound body tissue detecting device, ultrasound body tissue detecting method, and ultrasound body tissue detecting program |
| TWI584225B (zh) * | 2016-01-05 | 2017-05-21 | 財團法人工業技術研究院 | 皮膚組織估測方法及應用其之系統 |
| US10034653B2 (en) * | 2016-01-11 | 2018-07-31 | Biosense Webster (Israel) Ltd. | Tissue depth estimation using gated ultrasound and force measurements |
| CN106137251A (zh) * | 2016-07-15 | 2016-11-23 | 北京百思声创科技有限公司 | 用于皮下组织厚度测量的超声探头及测量仪 |
| WO2018029035A1 (en) * | 2016-08-08 | 2018-02-15 | Koninklijke Philips N.V. | A system and method for determining fat and lean body tissue components |
| CN106770647B (zh) * | 2016-11-17 | 2019-07-09 | 四川大学 | 脂肪含量测量系统及方法 |
| CN109009224A (zh) * | 2018-07-06 | 2018-12-18 | 北京工业大学 | 基于超声的皮下脂肪厚度测量仪 |
| US11911208B2 (en) * | 2018-08-21 | 2024-02-27 | The Government Of The United States, As Represented By The Secretary Of The Army | Systems and methods for the detection of fluid build-up resulting from an injury using ultrasound imaging |
| CN109864762A (zh) * | 2019-03-08 | 2019-06-11 | 北京工业大学 | 一种压力控制超声波的人体皮脂厚度测量仪 |
| CN110313938B (zh) * | 2019-08-01 | 2021-03-23 | 无锡海斯凯尔医学技术有限公司 | 皮下组织厚度测量方法、装置、设备及存储介质 |
-
2019
- 2019-08-01 CN CN201910706602.1A patent/CN110313938B/zh active Active
-
2020
- 2020-07-28 EP EP20847157.3A patent/EP4008263B1/de active Active
- 2020-07-28 WO PCT/CN2020/105022 patent/WO2021018108A1/zh not_active Ceased
- 2020-07-28 JP JP2022506602A patent/JP7249711B2/ja active Active
- 2020-07-28 BR BR112022001734A patent/BR112022001734A2/pt unknown
- 2020-07-28 US US17/631,103 patent/US12290399B2/en active Active
Also Published As
| Publication number | Publication date |
|---|---|
| JP7249711B2 (ja) | 2023-03-31 |
| JP2022543233A (ja) | 2022-10-11 |
| CN110313938B (zh) | 2021-03-23 |
| CN110313938A (zh) | 2019-10-11 |
| WO2021018108A1 (zh) | 2021-02-04 |
| EP4008263A1 (de) | 2022-06-08 |
| US20220273259A1 (en) | 2022-09-01 |
| US12290399B2 (en) | 2025-05-06 |
| EP4008263A4 (de) | 2023-01-25 |
| EP4008263C0 (de) | 2024-09-04 |
| BR112022001734A2 (pt) | 2022-04-12 |
Similar Documents
| Publication | Publication Date | Title |
|---|---|---|
| EP4008263B1 (de) | Verfahren zur subkutanen gewebedickenmessung, gerät und vorrichtung sowie speichermedium | |
| US10736522B2 (en) | Method and terminal for obtaining fetal heart | |
| US9445787B2 (en) | Systems and methods for capture and display of blood pressure and ultrasound data | |
| Jezewski et al. | A novel technique for fetal heart rate estimation from Doppler ultrasound signal | |
| JP7468201B2 (ja) | 生体検出装置、方法及びシステム | |
| JP6181176B2 (ja) | 母性心拍の改良された決定に関する方法及び胎児モニタリングシステム | |
| US9993226B2 (en) | Device and method for detecting skin to muscle depth by simultaneous detection of ultrasonic depth sensor and force sensor | |
| US12465326B2 (en) | Wearable non-invasive lung fluid monitoring system | |
| CN111110275A (zh) | 血管力学性能的测量方法、装置、系统及存储介质 | |
| EP2964099B1 (de) | Scannen zur identifizierung und begrenzung von stationären flüssigkeitspools | |
| US11583256B2 (en) | Fat layer dependent sensor adaptation | |
| US20210045709A1 (en) | Shear wave elasticity imaging method and ultrasonic imaging device | |
| JP6244724B2 (ja) | ストレスレベルを決定するための腎血流ドップラ信号の周波数領域分析変換 | |
| RU2789525C1 (ru) | Способ, аппарат и устройство для измерения толщины подкожной ткани и носитель данных | |
| US20100174187A1 (en) | Method and apparatus for determining hydration levels | |
| CN101410055B (zh) | 通过测量速度变化来确定水合程度的方法和装置 | |
| JP2022543248A (ja) | 心臓用装置 | |
| CN108720869B (zh) | 超声弹性测量方法及装置 | |
| CN117898766B (zh) | 血管成像方法、装置、电子设备及存储介质 | |
| CN119818089A (zh) | 一种超声多普勒血流检测仪的检测分析方法及系统 | |
| CN116584975A (zh) | 皮下组织厚度测量方法、装置、电子设备及存储介质 | |
| HK1124505A (en) | Systems and methods for capture and display of blood pressure and ultrasound data |
Legal Events
| Date | Code | Title | Description |
|---|---|---|---|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: THE INTERNATIONAL PUBLICATION HAS BEEN MADE |
|
| PUAI | Public reference made under article 153(3) epc to a published international application that has entered the european phase |
Free format text: ORIGINAL CODE: 0009012 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: REQUEST FOR EXAMINATION WAS MADE |
|
| 17P | Request for examination filed |
Effective date: 20220201 |
|
| AK | Designated contracting states |
Kind code of ref document: A1 Designated state(s): AL AT BE BG CH CY CZ DE DK EE ES FI FR GB GR HR HU IE IS IT LI LT LU LV MC MK MT NL NO PL PT RO RS SE SI SK SM TR |
|
| DAV | Request for validation of the european patent (deleted) | ||
| DAX | Request for extension of the european patent (deleted) | ||
| A4 | Supplementary search report drawn up and despatched |
Effective date: 20221223 |
|
| RIC1 | Information provided on ipc code assigned before grant |
Ipc: A61B 8/08 20060101ALI20221219BHEP Ipc: A61B 8/00 20060101AFI20221219BHEP |
|
| GRAP | Despatch of communication of intention to grant a patent |
Free format text: ORIGINAL CODE: EPIDOSNIGR1 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: GRANT OF PATENT IS INTENDED |
|
| INTG | Intention to grant announced |
Effective date: 20231115 |
|
| GRAJ | Information related to disapproval of communication of intention to grant by the applicant or resumption of examination proceedings by the epo deleted |
Free format text: ORIGINAL CODE: EPIDOSDIGR1 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: REQUEST FOR EXAMINATION WAS MADE |
|
| INTC | Intention to grant announced (deleted) | ||
| GRAP | Despatch of communication of intention to grant a patent |
Free format text: ORIGINAL CODE: EPIDOSNIGR1 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: GRANT OF PATENT IS INTENDED |
|
| INTG | Intention to grant announced |
Effective date: 20240419 |
|
| GRAS | Grant fee paid |
Free format text: ORIGINAL CODE: EPIDOSNIGR3 |
|
| GRAA | (expected) grant |
Free format text: ORIGINAL CODE: 0009210 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: THE PATENT HAS BEEN GRANTED |
|
| AK | Designated contracting states |
Kind code of ref document: B1 Designated state(s): AL AT BE BG CH CY CZ DE DK EE ES FI FR GB GR HR HU IE IS IT LI LT LU LV MC MK MT NL NO PL PT RO RS SE SI SK SM TR |
|
| REG | Reference to a national code |
Ref country code: GB Ref legal event code: FG4D |
|
| REG | Reference to a national code |
Ref country code: CH Ref legal event code: EP |
|
| REG | Reference to a national code |
Ref country code: IE Ref legal event code: FG4D |
|
| REG | Reference to a national code |
Ref country code: DE Ref legal event code: R096 Ref document number: 602020037278 Country of ref document: DE |
|
| U01 | Request for unitary effect filed |
Effective date: 20240911 |
|
| U07 | Unitary effect registered |
Designated state(s): AT BE BG DE DK EE FI FR IT LT LU LV MT NL PT RO SE SI Effective date: 20241001 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: NO Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241204 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: GR Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241205 Ref country code: PL Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: HR Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: ES Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 Ref country code: RS Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241204 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: RS Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241204 Ref country code: PL Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 Ref country code: NO Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241204 Ref country code: HR Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 Ref country code: GR Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20241205 Ref country code: ES Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: IS Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20250104 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: SM Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: CZ Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: SK Free format text: LAPSE BECAUSE OF FAILURE TO SUBMIT A TRANSLATION OF THE DESCRIPTION OR TO PAY THE FEE WITHIN THE PRESCRIBED TIME-LIMIT Effective date: 20240904 |
|
| PLBE | No opposition filed within time limit |
Free format text: ORIGINAL CODE: 0009261 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: NO OPPOSITION FILED WITHIN TIME LIMIT |
|
| U20 | Renewal fee for the european patent with unitary effect paid |
Year of fee payment: 6 Effective date: 20250630 |
|
| 26N | No opposition filed |
Effective date: 20250605 |